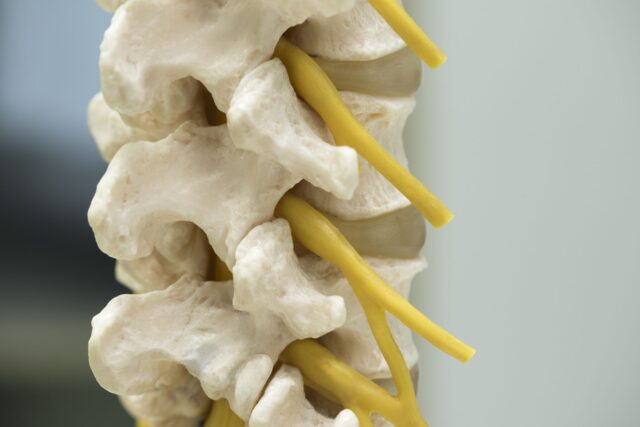
Percutaneous Discectomy
Percutaneous Discectomy is a minimally invasive procedure that can be performed with only local anesthetics and sedation and does not require any incisions, used to remove discuss material, therefore relieving pressure on a spinal nerve root that is causing a patient’s pain.
Frequently Asked Questions
Percutaneous Discectomy is an option for patients suffering from low back and leg (radicular) pain due to contained disc herniations, or protrusions. Typically patients have tried conservative management such as anti-inflammatory medications, physical therapy, and injection modalities such as epidural steroid injections and when surgical decompression is not indicated or planned. See Stryker’s home page for more information.
The procedure is done with local anesthetic at the introduction site. It will be performed entirely under x-ray (fluoroscopy) using a needle/ probe. By comparison, standard open discectomy can involve incisions of 1” and greater. After studying the annular boundaries of the disk by injection of contrast, the disc will be decompressed by aspiration of 1-2 cc of disc material using an auger inside of a channel.
Light conscious sedation may be used, as necessary, to help calm the patient. General anesthesia is not required (contraindicated).